Definition
Acrochordon (Skin tag): An epithelial outgrowth or protruding polypoid epithelial neoplasm.
Callosities: Hyperkeratosis of skin of hands or feet as a reaction to rubbing or to pressure over bony prominence. Focal involvement with clavus or com and more diffuse with callus.
DermatoRbroma: Small dome shaped fibrous nodules of brownish red color often at sites of skin prick puncture injury of extremities.
Hemangioma: Common soft tissue tumors of proliferating vessels: capillary, venous, or arterial with predilection for the head and neck. Most common are strawberry, cavernous, and cherry angioma.
Keloid scars: Excessive hypertrophic scar healing formation beyond wound edges.
lentigines (Solar): A brown pigmented, round, oval, or squarish, pigmented spot on the skin due to increased melanin from increased melanocytes at the epidermodermal junction. Most common on sun exposed skin.
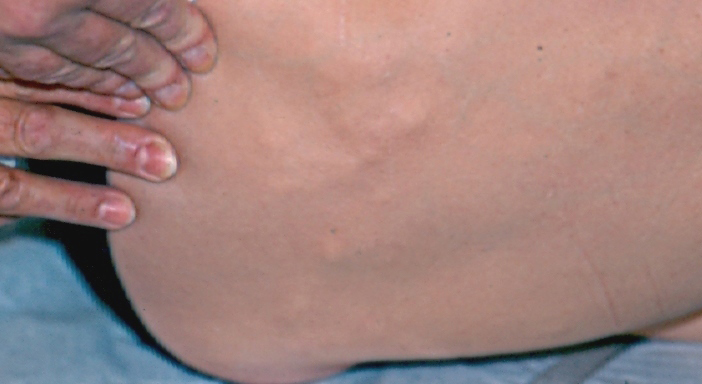
Lipoma: Benign tUmor of mature fat cells that are walled off or separated from sunrounding fat or other cells.
Nevi (Acquired melanocytic) or nevocytic: A common circumscribed stable malformation of the skin most likely arising from neural crest precursor cells such as the Schwann cell. or melanocyte. Differs from melanocytes by nest aggregations and having no dendriticlike processes. There are three forms: junctional, compound, and intradermal.
Pyogenic granuloma: A fungating, pedunculated growth related to capillary hemangioma.
Sebaceous hyperplasia: Oil or sebaceous glandular tissue growing at the skin surface.
Seborrheic keratosis: Benign epidermal tumor with hyperplasia of keratinocytes.
History
Symptoms
Acrochordon: Usually none, but may have itch or frank pain with torsion or rubbing irritation from clothes or another skin surface.
Callosities: Pressure sensitivity; thick and difficult to walk on.
Dermatofibroma: Asymptomatic dark, hard bumps of lower or upper legs, or arms. Occasional irritation and mild tenderness.
Hemangioma: Red spots and nodules in infancy, or tiny, red dots papules in adulthood.
Keloid scars: Large overgrowth of hard skin after healing of a wound or skin injury (e.g., insect bites, acne papules, skin piercing for earrings, or surgery).
lentigines (Solar): Painless brown spot on arms, face, legs, chest, or back usually on sun exposed surfaces.
Lipoma: Soft lumps growing under skin of neck, trunk, and extremities. May be small or large.
Nevi (Acquired melanocytic) or nevocytic: Painless, clear, tan, light and dark brown spots and papules in any skin location.
Pyogenic granuloma: Fast growing, easily injured reddish growth on skin or mucous membranes.
Sebaceous hyperplasia: Slow growing, small white bumps. Mainly affects the face.
Seborrheic keratosis: One or more ;stuck on; (;warts or moles;) appearing lesions which are tan, brown, or black. May be slightly roughish or raised.
Age
Acrochordon: Rare in childhood, usually in middle and old age. Occasional before 30. Mostly in females.
Callosities: Any, but not common in childhood.
Dermatofibroma: Any, but usually adults, more often females.
Hemangioma: Congenital for strawberry and cavernous and over 20 is usual for cherry angiomas.
Keloid scars: Any age, sex, or nationality.
lentigines (Solar): Usually greater than 30 years, males and females. Lipoma: Adult, chiefly in the late or middle decades; may occur younger with the familial form.
Nevi (Acquired melanocytic) or nevocytic: Childhood to 90 years.
Pyogenic granuloma:Any.
Sebaceous hyperplasia: Adult, middle, and old age.
Seborrheic keratosis: Extremely rare in children, may occur in young adults and is common in the elderly.
Onset
Acrochordon: Tiny tags of skin, with chronic growth in both size and number.
Callosities: Chronic, with repetitive rubbing, especially in the hands or over the bones of the feet.
Dermatofibroma: Noticed suddenly, but is a lesion of chronic, slow progression.
Hemangioma: Occurs congenitally or sudden in early infancy (1 in 200) with chronic growth. Cherry angiomas occur suddenly to chronically in adults.
Keloid scars: Chronic. Overgrowth may follow healing of an injury by weeks or months, but some itch or irritation often persists. History of significant skin injury may be vague.
lentigines (Solar): Chronically, occurring any time after age 30 and increasing in size and number.
Lipoma: Sudden to chronic.
Nevi (Acquired melanocytic) or nevocytic: Chronic.
Pyogenic granuloma: Acute with small red papule.
Sebaceous hyperplasia: Gradual, chronic.
Seborrheic keratosis: Chronic, slow growing.
Duration
Acrochordon: Indefinite and permanent.
Callosities: Indefinite, but tend to diminish as pressure and rubbing cease.
Dermatofibroma: Indefinite to permanent.
Hemangioma: Strawberry marks tend to regress after age 6 months to 1 year and become up to 95 percent resolved in 7 to 8 years. Cherry angiomas tend to be permanent. Cavernous resolve to some degree in 7 to 10 years as well.
Keloid scars: Indefinite, permanent.
lentigines (Solar): Permanent without treatment.
Lipoma: Indefinite to permanent.
Nevi (Acquired melanocytic) or nevocytic: Many years, peaking in twentieth years, fading by ninetieth year.
Pyogenic granuloma: Indefinite, longterm.
Sebaceous hyperplasia: Permanent, long term.
Seborrheic keratosis: Permanent with slow growth and increasing pigment.
Intensity
Acrochordon: Single local to numerous, widespread.
Callosities: From single, small eraser size pressure points to involvement of the entire heel and foresoles due to tight, pinching foot wear.
Dermatofibroma: Usually singly or in pairs.
Hemangioma: From single, small strawberry nodules and small, deeper cavernous nodules to large disfiguring nodules. Cherry angiomas tend to be multiple and widespread in adults.
Keloid scars: Single, small overgrowth to involvement of every truncal acne lesion. May be a very exaggerated overgrowth onto normal skin compared to the small size of injury.
lentigines (Solar): Range from single, few mm lesions to many, up to 1 to 2 cm. lipoma: Single, range from I to 2 em lesions to many lesions as large as several centimeters.
Nevi (Acquired melanocytic) or nevocytic: One lesion to several, beginning any time after birth and peaking in mid twenties, to maximal number of 30 to 40 lesions. Some lesions tend to flatten by 40 years of age and many disappear by age 90.
Pyogenic granuloma: Starts small but grows rapidly over few weeks. Usually single lesions. Ulceration and inflammation is common.
Sebaceous hyperplasia: One to many lesions, typically 1 to 5 mm in diameter
Seborrheic keratosis: One to numerous on trunk, head, extremities. Never the palms or soles.
Aggravating Factors
Callosities: Continued manual labor for hands and continued footwear that presses or rubs tightly.
Dermatofibroma: Further skin injury.
Keloid scars: Scratching, rubbing.
lentigines (Solar): Intense sun exposure.
Pyogenic granuloma: Onset often follows minor trauma. Bleed easily with minor injury. Conservative treatment often leads to recurrence of one or more.
Seborrheic keratosis: Sun damage leads to increased risk. Hemangioma/ Acrochordon/lipoma/Nevi (Acquired melanocytic)/ Sebaceous hyperplasia or
Nevocytic: No aggravating factors.
Alleviating Factors
Acrochordon: Removal.
Callosities: Cease manual labor using the hands and obtain new better fitting or custom made shoes.
Dermatofibroma: Removal.
Hemangioma: Tincture of time for most strawberry and cavernous type.
lentigines (Solar): Appropriate treatment.
Nevi (Acquired melanocytic) or nevocytic: Time, many fade by age 90.
lipoma/Keloid scars/Pyogenic granuloma/Sebaceous hyperplasia/ Seborrheic keratosis: No alleviating factors except removal.
Associated Factors
Acrochordon: Hereditary propensity.
Callosities: Chronic pressure, genetic predisposition.
Dermatofibroma: Occasional history of bite or prick injury preceding the lesion.
Hemangioma: Hereditary predilection. Not uncommon for family members to have or had similarly located hemangiomas.
Keloid scars: More predilection in dark skinned individuals, especially on the jawline and ear lobes. Some familial predilection.
lentigines (Solar): Familial predisposition; largest and more numerous in late years.
Lipoma: The familial form is characterized by many small truncal and extremity lesions.
Nevi (Acquired melanocytic) or nevocytic: No known external effects, so presumed to be of hereditary origin.
Pyogenic granuloma: Equal in both sexes.
Sebaceous hyperplasia: Hereditary propensity, oily skin, and/or acne history is common.
Seborrheic keratosis: Hereditary predilection. Some tumor associated factors may also playa role.
Physical Examination
General: Skin.
Acrochordon: Soft, fleshy to tan or brown polyps of skin from less than 1 mm to 1 or 2 cm. Found on neck, chest, axillae primarily, but are also common on the inside top of the thighs. More prevalent in the obese and females.
Callosities: Thick, yellowish, opaque, tough hard, hyperkeratotic skin. Located around the heels, under and around the toes, foresoles of the feet, and over the palmer metacarpophalangeal joints of the hands. Sometimes pain on pressing on thicknesses.
Dermatofibroma: 1 cm or less brownish reddomed nodule on an extremity. Non tender and typically dimples with bilateral compression.
Hemangioma: Bright red macule that may be elevated and almost nodular in first 6 to 12 months. Very discrete sharp bordered. Located on the neck or head (including the face) for strawberry nevus (hermangioma). Deeper nodular fullness with irregular bright red and white color, or fleshy surface over deep, bruise like reddish purple nodule, which is often compressible. Size varies from 1 to 2 cm to several centimeters for cavernous type. Cherry angiomas are red to purpledomed papules of a few millimeters in diameter. Found on trunk and extremities.
Keloid scars: Thick, fibrous, fleshy, red or brown lesions seen over grown hyperplastic scars. Most common on ear lobes (after piercing), jaws and chest, shoulder or upper back (after acne), and any site of surgery.
lentigines (Solar): Asymptomatic irregular brown macule with sharp borders from a few millimeters to a couple centimeters in diameter; Roundish, oval, square shapes on areas of chronic sun exposure.
Lipoma: Soft, subcutaneous, poorly marginated mobile mass 1 to many centimeters located on the neck, trunk, or extremities. Rarely tender to pressure.
Nevi (Acquired melanocytic) or nevocytic: Classified as junctional, compound and intradermal.
Junctional: Usually 2 to 6 mm darkly Pigmented macules with flat or slightly raised hairless surface borders.
Occur anywhere on the body. Compound: Three to 5 mm in diameter tan, flesh-colored to reddish, moderately pigmented and slightly raised, to papillomatous. Occur with hairs on any area of body.
Intradermal: May be larger than junctional or compound nevocytic nevi. Dome shaped or very papillomatous without evident pigment or tan, brown, or reddish coloration. Frequently Occur where hairs grow on any body area.
Pyogenic granuloma: Friable, 1/2 to I cm red, violaceous sessile or polypoid papule on any skin surface. Occur singly.
Sebaceous hyperplasia: Small, whitish yellow umbilicated, tiny ringed papules of face. One to many in number.
Seborrheic keratosis: Fleshy yellow, pink, tan, brown, or black sharply demarcated “stuck on” looking raised lesion. Associated with a waxy, velvety, scaly, or stipled surface. Ovalish to roundish appearance on the trunk, head, extremities, or anywhere except the palms and soles. Single to numerous in number tend to achieve greater thickness and darker pigment on scalp and trunk.
Pathophysiology
Acrochordon: Covered by flat or hyperplastic epithelium and loose collagen with no true signs of neoplasm in dermis.
Callosities: Reactive epithelial hyperkeratosis without neoplastic change.
Dermatofibroma: Lesions contain fibroblasts and histrocytes that may contain hemosiderin and lipids. This merges with the dermis and entraps collagen.
Hemangioma: strawberry hemangioma: Very cellular with packed spindle cells surrounding vascular lunina. Mitoses is often prominent until regressive stages, when they decrease, endothelium flattens and connective tissue proliferates. Cavernous hermangiomas: Dilated large vessles with flattened endotheluim. Wall may be thickened from fibrosis and inflammation. Cherry hemangiomas: Small dilated vessles in superficial dermis, covered by flattened epitheluim.
Keloid scars: Broad, hyalinized appearing branched bands of irregular collagen.
lentigines (Solar): Increased melanocytes in darkly pigmented basal cells with elongated, budded, or club shaped rete ridges.
lipoma: Tumor of well circumscribed, mature adipose tissue. Always benign.
Nevi (Acquired melanocytic) or nevocytic: All have nests of uniform nevus cells or theques. Junctional cells are found in lower epidermis and contain melanin. Compound nevus cells are located in nests of the lower epidermis and high dermis. Intradermal nevus cells are located in nests in the papillary and reticular dermis.
Sebaceous hyperplasia: Normal sebaceous gland tissue in grape-like clusters, surrounding wide sebaceous duct, giving the umbilicated appearance at the skin surface. These glands are normally in the dermis.
Seborrheic keratosis: Hyperkeratosis in thickened epidermis with increased melanin. Melanosome macrocomplexes are found in the various cells of the skin.
Diagnostic Studies
Laboratory: Not applicable.
Radiology: Not applicable.
Other: Biopsy should be performed on any suspicious lesion in which the diagnosis is uncertain. Biopsies can be performed by punch, excisional, or needle techniques. Acrochordon can be confused with papilloma. Nondysplastic acquired nevi can turn into melanoma but the risk is very low. Pyogenic granuloma may be clinically similar to amelanotic melanoma.
Differential Diagnosis
Traumatic
Acrochordon: May be confused with keloid.
Dermatofibroma: Scar is not as pigmented or has a diffuse, merged border.
Hemangioma: Hematomas and ecchymoses follow a history of contusion or injury, are more acute and self limited, and change colors from the violaceous to blue, green, yellow, brown.
Keloid scars: Hypertrophic scar is overgrowth of normal healing skin that does not overgrow excessively; diminishes with time.
lentigines (Solar): Postinflammatory hyperpigment or residual hemosiderin after bruise has a more even, consistent pigment and more diffuse border that fades lighter, especially without sun.
lipoma: Hematoma is more firm and dark in color-bluish. Sometimes tumorous isolation of fat is caused by contusion-compression injury to fatty tissue.
Nevi (Acquired melanocytic) or nevocytic: A bruise is diffuse and of a different color. Hemosiderin deposit is also diffuse and obviously more superficial than nevi. Hemosiderin is always flat, even, dark tan or brownish.
Callosities/Pyogenic granuloma/Sebaceous hyperplasia/Seborrheickeratosis: Not applicable.
Infectious Callosities: Occasionally there are underlying warts leading to a reactive hyperkeratosis.
Hemangioma: More inflammation and symptoms with carbuncles and abscesses, as well as acute onset and short, self-limiting course.
lipoma: Abscess is usually inflammed, tender, more indurated and fluctuant.
Acrochordon/DermatoFibroma/Keloid scars/Lentigines (Solar)/Nevi (Acquired melanocytic) or nevocytic/Pyogenic granuloma/Sebaceous hyperplasia/Seborrheic keratosis: Not applicable.
Metabolic
Acrochordon: Neurofibroma is more sessile, of a larger size, and more firm and fixed.
Hemangioma: Kaposi sarcoma is of lymphatic endothelial origin and are violaceous or brown/red macules, papules, or nodules. Seen mostly on legs and progress proximately. Usually occur as multiple lesions and are common on face, head, and chest. Commonly associated with human immunodeficiency virus.
Sebaceous hyperplasia: Xanthoma is a broad, flat, whitish yellow plaque with even, discrete borders.
Callosities/Dermatofibroma/Keloid scars/Lipoma/Lentigines (Solar)/ Nevi (Acquired melanocytic) or nevocytic/Pyogenic granuloma/ Seborrheic keratosis: Not applicable.
Neoplastic Acrochordon: Branchial cysts are usually deep purplish red and arise on the upper neck in the second or third decade of life.
Dermatofibroma: Basal cell carcinoma is usually not as pigmented, as brownish, or as firm; not as common on the legs.
Lentigines (Solar): Care-au-lait spots: Single or multiple, 1.5 cm and greater, with sharp very finely irregular borders with an even tan. Increased numbers associated with neurofibromatosis.
Simple lentigo: Usually just a few millimeters in diameter, light brown to jet black. More like a junctional nevus. Onset common in childhood. Not necessarily photodistributed.
Nevi (Acquired melanocytic). or nevocytic: For melanoma see under section Premalignant and Malignant Neoplasms. Dysplastic nevus syndrome: Familial tendency. Often with melanoma history in family or patient. Tend to be more oval and larger (greater than 6 mm) man acquired nevi. They tend to have more red coloration along with color variation in single lesions. Individual lesions vary in color, size, and shape and borders tend to meld diffusely into surrounding skin. Most prevalent on trunk and extremities and sun exposed surfaces. May be few to over a hundred. Any new, changing or questionable lesion should be biopsied for melanoma.
Pyogenic granuloma: Amelanotic melanomas are usually much slower growing less friable, more domed and sessile than pedunculated. For the more hyperkeratotic skin ringed lesions, biopsy is the definitive measure.
Sebaceous hyperplasia: Basal cell carcinoma is usually larger with translucent rolled borders and telangiectasias (tiny, fine red surface vessels.) Often leave ulcerations.
Seborrheic keratosis: Cafe-au-lait remain flat and even tan color, usually much larger. Increased numbers associated with neurofibromatosis.
Melanomas: Are less distinct, with diffuse borders and more irregularity in shape, color, and elevation.
Callosities/Hemangioma/Keloid scars: Not applicable.
Vascular
Acrochordon: Pyogenic granuloma: Is eroded, blood red, and friable over widerspread area.
Hemangioma: Pyogenic granuloma: More polypoid than the above angiomas. Ulceration and inflammation are common. Affect all ages.
Arteriovenous hemangiomas: Bluish red papules with small nodules in adults, with thin-walled dilated veins and arteries in deeper areas.
Venous lakes: Violaceous, blue, small-domed papules usually of the elderly. Occur on the lips or exposed skin. Blanch completely with pressure.
Keloid scars: Hemangioma or pyogenic granuloma more reddish blue vascular and not as firm.
Lipoma: Deep cavernous hemangiomas or large varicosities: Would have some bluish red, purple discoloration, even in subcutaneous tissue.
Nevi (Acquired melanocytic) or nevocytic: Hemangiomas are blood red or purple with no melanin.
Pyogenic granuloma: Other hemangiomas are less sessile, less protruding and rarely pedunculated. Also less susceptible to trauma.
Callosities/Dermatofibroma/lentigines (Solar}/Sebaceous hyperplasia/Seborrheic keratosis: Not applicable.
Congenital
Hemangioma: Port-wine stains or nevus flammeus are large, red to purple, broad vascular disorders, associated with congenital syndromes. Cover wide, multiple centimeter areas, usually in nerve distribution. Occur unilaterally on the face or trunk.
lentigines (Solar): Congenital nevi: Approximately a 1 percent Occurrence rate at birth. Raised, not macular and often hairy, darkly pigmented.
Nevi (Acquired melanocytic) or nevocytic: Congenital nevi: Occur in approximately 1 percent of births. They are nearly always larger than other melanocytic or nevocytic nevi (1.5 cm to greater than 20 cm). The giant or bathing trunk nevi have very irregular borders and surfaces, with brown to black pigment and tend to grow hair. Medium and smaller congenital nevi share similar characteristics but are not as grossly irregular. These nevi can undergo malignant change, but the risks are controversial. Suspicious and changing lesions should be biopsied.
Acrochordon/ Callosities/Dermatofibroma/Keloid scars/Lipoma/ Pyogenic granuloma/Sebaceous hyperplasia/Seborrheic keratosis: Not applicable.
Acquired
lentigines (Solar}: Nevi: Usually have at least some palpability, less discrete borders, are usually round, with some decreasing by age 40.
Nevi (Acquired melanocytic) or nevocytic: Becker’s nevi: Are generally large, unilateral hyperpigmentations growing hair. Common on shoulders of prepubescent boys. More faint with less hair on varied body sites, usually in dermatomes of the trunk. Irregular tan macules.
Spitz nevi: Are sharply circumscribed and distinctive pink, orange, or red in lesions. Common on face of children, but can be found elsewhere. Occur in adolescents and occasionally in adults. Characteristic histologically but are sometimes difficult to separate from melanoma. They should be excised for biopsy.
Halo nevi: Are typical nevocytic-melanocytic nevi with a surrounding zone of depigmentation. Are benign and likely undergoing immune system attempt to eradicate.
Mongolian spots: Are bluish black, ovoid, or roundish pigment patches. Usually occur on the sacrum of Black and Oriental babies. Often fade with time and are benign.
Nevi of ota and ito: Are patches of bluish melanocytosis like mongolian spots, but ota’s nevi are found unilaterally in trigerrninal nerve distribution of the face. Involve the ocular structures as well as the skin.
Nevi of Ito involve the neck, arm, or shoulder unilaterally. Both may be present at birth. Both more common in Asians. No treatment required.
Sebaceous hyperplasia: Fordyce spot: Is ectopic sebaceous glands appearing as tiny, whitish yellow, visible but barely palpable dots, in broad groupS on the lips or genitalia.
Seborrheic keratosis: Solar lentigo: Hard to distinguish early but benign. Usually not as distinctly “stuck on” and has a more uniform, smooth, tan, brown color.
Acrochordon/ Callosities/Dermatofibroma/Hemang ioma/Keloid scars/Lipoma/Pyogenic granuloma: Not available.
Treatment
Acrochordon: Simple excision tangentially or with electrosurgery, using lidocaine 1 to 2 percent as a local anesthetic.
Callosities: Parring with surgical blade or application of keratolytics (e.g., salicylic acid plasters). The mechanical irritation must be alleviated with padding, better-fitting shoes, etc.
Dermatofibroma: None or deep cryosurgery unless there is a question of basal cell carcinoma then simple excisional biopsy.
Hemangioma: For strawberry and cavernous hemangiomas in infancy, document by photography and follow for the first year unless the lesion interferes with vital structure or function. May take up to 7 years to regress. If intervention is indicated, start with triamcinolone 5 mg/ml intralesional injections at 3 to 5 week intervals.
Cherry angiomas require no treatment but can be ablated with electrosurgery.
Keloid scars: Scar revision or excision may help, but there is a significant risk of recurrence. Best to initiate intralesional injections of triamcinolone 1 mg/ml every 3 to 5 weeks, observing for shrinkage and softening. Dose can be increased as indicated to 40 mg/ml. Constant pressure by bandaging has shown some shrinkage capability. Silastic gel sheating taped over the keloid to totally cover the lesion and is left in place for 12 of every 24 hours, has been beneficial. (Controversial due to silicone/silastic safety issue.)
Lentigines (Solar): Usually no treatment is required except for cosmetic purposes. Cryosurgery with liquid nitrogen for light blister peel, light electrodessication, or light acid peel can remove or diminish the lesion.
Lipoma: Necessary only if there are nerve pressure symptoms, cosmetic, or functional problems. Surgical excision can be performed in these Instances using local or field block infiltration anesthesia.
Nevi (Acquired melanocytic) or nevocytic: None necessary but are frequently removed for cosmetic reasons or chronic irritation.
Pyogenic granuloma: Excised using narrow margin, sharp excision, electrocautery, or tangential excision with deep electrodessication and currettage. Too shallow or conservative removal may lead to return, sometimes with satellites.
Sebaceous hyperplasia: For numerous unsightly lesions isotretinoin (Accutane) is used at 40 mg. One to 2 times daily pending size and weight for 4 months. Cryosurgery with liquid nitrogen or electrodessication is also effective.
Seborrheic keratosis: Removal by cryosurgery, currettage, flat excision (full-thickness or shave) or a combination.
Pediatric Considerations
Lipoma: Rare in pediatrics and there are no obstetrical considerations. Can usually wait until postpartum.
Pyogenic granuloma: Same as adults.
Obstetrical Considerations
Nevi (Acquired melanocytic) or nevocytic: Moles or nevi tend to develop or change during pregnancy.
References