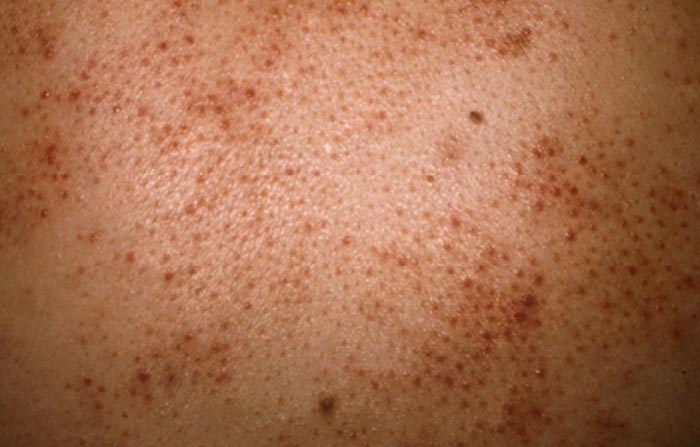
There are several variants of eosinophilic folliculitis, which is also known as ‘eosinophilic pustular folliculitis’ or ‘Ofuji disease’. The name is due to skin biopsy finding of eosinophils (a type of immune cell) around hair follicles.
Eosinophilic folliculitis (EF) is an idiopathic, extremely pruritic, papular follicular eruption of the upper trunk, face, neck, and proximal extremities occurring in advanced HIV disease and/or after initiation of highly active antiretroviral therapy, often associated with peripheral eosinophilia. EF occurring in HIV disease is different from that of Ofuji’s disease.
Causes of Eosinophilic Folliculitis
Unknown.
Symptoms of Eosinophilic Folliculitis
The signs and symptoms of folliculitis vary, depending on the type of infection. In superficial forms of the disorder, small pimples develop around one or more hair follicles
Diagnosis
Clinical diagnosis confirmed by skin biopsy, with cultures ruling out infectious causes. A new primary lesion (follicular papule) should be marked with a pen and biopsied with a 2-mm punch.
Treatment
Pruritus is moderate to severe, significantly affecting quality of life. Changes secondary to chronic scratching such as secondary infections and lichen simplex chronicus also should be identified and treated. The most predictably effective therapy is a short tapered course of oral glucocorticoid such as prednisone.
Antihistamines Those causing sedation are more effective for symptomatic relief of pruritus. Doxepin, 10-100 mg, is especially effective at bedtime.
Topical Agents
- Glucocorticoids Class I (superpotent) glucocorticoids applied to affected areas produce fair to moderate improvement in pruritus and lesions. Patients using these agents on the face should be closely monitored for atrophic changes.
Systemic Agents
- Prednisone Initial dose of 70 mg, followed by a taper of 5-10 mg/d (14 – 7 days) provides rapid symptomatic improvement as well as resolution of EF. EF gradually recurs after completion of course.
- Isotretinoin (Accutane) 1-2 mg/kg/d (about 80 mg) very effective in causing resolution of EF. Once symptoms and skin findings have resolved, dose is reduced to 40 mg/d for 2-4 weeks and then tapered to 40 mg qod. Dosing may be discontinued in 1-2 months if symptoms do not recur. Many HIV-infected individuals treated with HAART have elevated triglyceride levels; isotretinoin can further increase triglyceride levels.
- Itraconazole 400 mg/d for 4 weeks reported to be effective.
Phototherapy
- UVB Treatments are usually given three times a week, tapering as symptoms of EF resolve. Moderately effective.
- Natural sunlight Many individuals cannot tolerate natural sunlight because of treatment with photosensitizing drugs such as trimethoprimsulfamethoxazole (Bactrim), which are photosensitizing in the UVA spectrum.
References